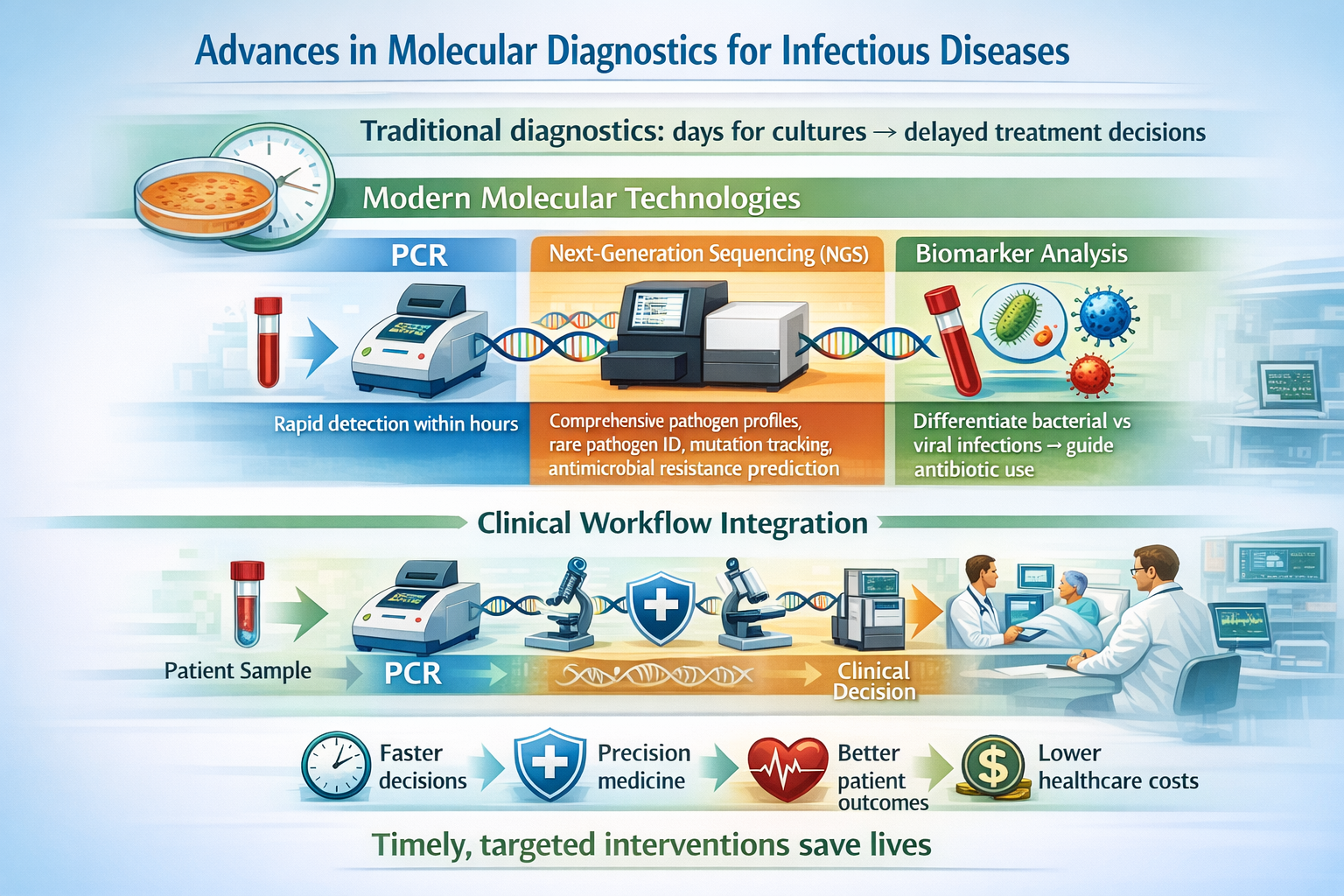
Molecular diagnostics have revolutionized the detection and management of infectious diseases, addressing one of modern medicine’s greatest challenges: identifying the cause of infection quickly and accurately. Traditional diagnostic methods often required days for bacterial or fungal cultures to grow in the laboratory, delaying treatment decisions. In contrast, recent advances in molecular technologies—such as Polymerase Chain Reaction (PCR), DNA sequencing, and biomarker identification—have transformed clinical practice by enabling rapid, precise, and comprehensive pathogen detection. PCR remains a cornerstone in clinical diagnostics, capable of detecting minute quantities of pathogen genetic material within hours. Next-Generation Sequencing (NGS) has further expanded diagnostic capabilities by providing complete genomic profiles of infectious agents. This allows clinicians to identify rare pathogens, monitor viral mutations, and predict antimicrobial resistance from a single patient sample. Biomarker analysis adds another dimension, leveraging signals from the host immune response to distinguish between bacterial and viral infections, thereby guiding appropriate antibiotic use and supporting early diagnosis and treatment stratification. The integration of these technologies into routine clinical workflows has significantly improved diagnostic accuracy, accelerated therapeutic decision-making, and enhanced patient outcomes, particularly in critical care settings. While challenges remain—such as cost, data interpretation, and infrastructure requirements—ongoing innovations and increasing accessibility are expected to broaden their impact. By transitioning these tools from specialized research laboratories into everyday hospital practice, molecular diagnostics are driving the emergence of precision medicine for infectious diseases. Ultimately, these advances reduce hospital stays, lower healthcare costs, and, most importantly, save lives by ensuring timely and targeted interventions.
December 28, 2025